Ovarian Cancer
The key to successfully treating ovarian cancer is accurate detection, expert diagnosis, personalized treatment options, and survivorship support for every patient. At Saint Luke's Cancer Institute, our multidisciplinary team provides comprehensive care for patients with ovarian cancer.
Why choose us?
Our gynecological oncologists follow a patient through every step of treatment.
Our program features:
- Medical oncologists and hematologists who subspecialize in ovarian cancer
- Access to more than 200 National Cancer Institute-sponsored clinical trials and industry-led studies through our agreement with the internationally recognized Washington University School of Medicine
- Genomic sequencing and precision oncology services for advanced cancers
- Nurse navigators who serve as patient resources and advocates through treatment and beyond
- Supportive Oncology and Rehabilitation Services program to help patients overcome the physical and emotional challenges that often follow diagnosis and treatment
What is ovarian cancer?
Cancer happens when cells in the body change (mutate) and start to grow out of control. These cells can form lumps of tissue called tumors. Cancer that starts in the ovaries is called ovarian cancer. Ovarian cancer can spread from the ovaries to other parts of the body. This spread is called metastasis. The more cancer spreads, the harder it is to treat.
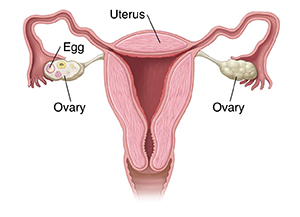
Understanding the ovaries
The ovaries are a pair of walnut-sized organs in the pelvis of a person assigned female at birth. They're part of the reproductive system.
The ovaries are on either side of the uterus. The uterus is the organ that holds the baby during pregnancy. Ovaries hold and release the eggs that, when joined with sperm, can grow into a baby. The ovaries also make the hormones progesterone and estrogen.
When a person reaches menopause, the ovaries stop releasing eggs and stop making certain hormones.
When ovarian cancer forms
There are three different main types of ovarian cancer:
- Epithelial tumors. These start in the cells that cover the outer surface of the ovaries. This is the most common type of ovarian cancer. The most common subtype of epithelial tumors are high-grade serous.
- Germ cell tumors. These start in the cells inside the ovary that make the eggs. These rare tumors are most common in people in their teens and early twenties. There are different subtypes of germ cell tumors.
- Stromal tumors. These start in support cells that hold the ovaries together and make female hormones. This is a rare form of ovarian cancer.
Treatment choices for ovarian cancer
You and your healthcare provider will decide on the treatment plan that's best for you. Treatment choices may include:
- Surgery. This is often done to remove the ovary with cancer or both the ovaries, along with nearby tissue and organs. Sometimes the uterus is removed (hysterectomy) as well. If the cancer has spread, the surgeon will try to remove as much of it as possible. This is called debulking surgery.
- Chemotherapy (chemo). This uses strong medicines to kill cancer cells. Chemo is often used along with surgery. It can be given before or after surgery.
- Targeted therapy. This might be used for more advanced ovarian cancer. These medicines target specific changes in the genes or proteins in or on the cancer cells to kill them while sparing normal cells.
- Immunotherapy. This uses medicines to help the body's own immune system to fight cancer.
- Hormone therapy. This can help treat stromal tumors. It blocks the hormones that help these tumors grow.
- Radiation therapy. This is rarely used to treat ovarian cancer. It uses focused high-energy X-rays to kill cancer cells.
- Clinical trials. These are research studies to test new ways of treating cancer. Ask your healthcare provider if a clinical trial is a choice for you.